The brain is the control centre of the human body. Our brains contain a network of approximately 100 billion neurons linked to each other by trillions of connections called synapses. In conjunction with the spinal cord, commonly referred to as the ‘information highway’, it forms the central nervous system (CNS). The CNS is responsible for transporting messages to and from all parts of the body.
The brain processes our thoughts and information about our environment and controls voluntary and involuntary functions. To perform this heavy lifting, itn needs an uninterrupted supply of nutrients to feed billions of cells that make up the CNS. In fact, our brains comprise just 2% body mass, but consume 20% of cellular oxygen and receive 15% cardiac output. Glucose is the major oxidative fuel of the brain. Thus, proper brain function is closely tied to metabolism and metabolic health.
What is Metabolism?
Metabolism occurs in every cell in the body. It is a series of chemical processes in each cell, transforming the calories we eat into fuel to keep us alive. These processes sustain life, everyday functioning and include breaking down food and drink to energy and building or repairing our bodies.
What is Metabolic Health?
Metabolic health is described as having ideal levels of blood sugar, triglycerides, high-density lipoprotein (HDL) cholesterol, blood pressure and waist circumference, without using medications.
Cerebral metabolic rate (CMR) can be expressed in terms of oxygen (O2) consumption of the brain. An average brain weighing 1400g consumes 49ml of O2 per minute, 20% of the total metabolic rate of the body (250ml O2/min).
To achieve oxidation within brain cells, O2 needs a substrate. Enter glucose, the primary substrate for cerebral metabolism. To measure substrate utilisation, we calculate the CMR of glucose (glc). The ratio of CMR (O2) / CMR (glc) is known as the oxygen-glucose index (OGI). When no other substrates are metabolised, complete oxidation of glucose produces an OGI close to 6.0 (theoretical maximum). Studies have found that global OGI varies from around 5.5–6.0 in animal and human brains.
Consequently, the majority of brain function is driven by glucose — from cellular maintenance (neuronal and non-neuronal) and oxidative stress management to the production of adenosine triphosphate (ATP). ATP is an energy-storing molecule that drives cellular metabolism and synthesises neurotransmitters (essential for relaying messages). Glucose reaches the brain via glucose-transporting cells, GLUT3. However, disruption of glucose pathways, delivery and metabolism leads to debilitating brain disease.
Learn more about the brain and metabolic heath here.
What is Encephalopathy?
Encephalopathy is a general term for any disease or damage to the brain that alters its function or structure. Encephalopathies are a group of disorders characterised by several causes, including but not limited to infectious microorganisms, long-term (LT) exposure to toxins, increased pressure in the skull, lack of oxygen or blood flow to brain, poor nutrition and metabolic and mitochondrial dysfunction. Encephalopathies are classified as either irreversible or reversible. Listed below are examples of commonly observed encephalopathies:
Irreversible
- Chronic Progressive Trauma (CPT): This is caused by repeated injuries to the head. Over time, these injuries cause brain damage. It’s most commonly found in athletes competing in contact sports, such as football, boxing or ice hockey. Several injuries lead to a build-up of tau, a protein that ordinarily stabilises brain cells. Excess tau caused by recurrent injuries clumps together and kills neurons. It eventually spreads to other parts of the brain and inhibits proper functioning.
- Hypoxic-Ischemic Encephalopathy (HIE): This is an inborn complication affecting full-term infants. As its name suggests, HIE results from a hypoxic (oxygen deficiency) and ischemic (inadequate blood supply) event(s) during pregnancy, leading to inflammation, oxidative stress and eventually causing brain damage in the foetus. Impaired blood and oxygen delivery to the brain cause 60% of infants to die or have several disabilities by the age of two. Disabilities include mental retardation, epilepsy and cerebral palsy. Very few preventative treatments exist, but studies are focused on managing disabilities to improve the outcome of infants with HIE.
Reversible
- Brain tumours: These can be benign or malignant. Benign tumours, although not aggressive, can harm cells and tissue around them causing inflammation and increased pressure inside the skull. Malignant tumours are cancers that quickly invade surrounding tissue and cause damage to the CNS. Provided it is safe, surgical removal of the tumour is the preferred option to relieve patients. If the tumour resides in a sensitive region of the brain, chemotherapy or radiation is prescribed to shrink and kill the tumour. Radiation therapies kill cancer cells but also damage surrounding healthy tissue. Loss of faculties such as physical strength, motor skills, balance and speech may result; patients must undergo rehabilitation to regain these.
- Hashimoto’s encephalopathy: A rare disorder, believed to be autoimmune, whereby antibodies mistakenly target the thyroid tissue. Presence of antithyroid antibodies is an indicator of an improperly functioning immune system. Encephalopathy occurs due to an abnormal response from the immune system in response to an infection or trigger. In patients, it is characterised by impaired brain function; patients exhibit an altered mental state. Severity and symptoms vary widely, however corticosteroids are prescribed to ease the disorder.
- Hepatic encephalopathy (HE): HE is usually associated with advanced liver disease due to improper functioning of the liver. Toxins aren’t filtered by the liver and enter the bloodstream, making their way up to the brain. Hepatic encephalopathy can also result from infections, lack of water, internal bleeding or excessive alcohol consumption.
- Infections of Brain: These are usually caused by bacteria. Examples include sepsis, meningitis or a urinary tract infection. Sepsis occurs when the body has an unusually severe response to an infection. The immune system releases chemicals into the bloodstream, causing inflammation, clots, drop in blood pressure and organ failure. Meningitis is a rare infection that affects the meninges (membranes) that protect the brain and spinal cord. If not treated quickly, meningitis causes brain damage. Urinary tract infections and others have been identified as potential stroke triggers.
- LT exposure to toxins: This includes intoxication from drugs, solvents, radiation, paints, chemicals and some metals. Accidental (or intentional) ingestion of substances such as carbon monoxide, ethanol, methanol, toluene and opioids lead to cognitive impairment.
- Metabolic encephalopathy (ME): This includes disorders of the brain caused by underlying illness such as diabetes, liver disease, heart or renal failure. MEs are unrelated to any structural brain abnormality. As symptoms and causes are varied, ME is a clinical state, not a diagnosis. Further testing must be conducted to determine and treat the underlying condition.
Symptoms differ across the various types of encephalopathies. The National Institute of Neurological Disorders and Stroke (NINDS) outlines common symptoms:
- Cognitive ability loss
- Inability to concentrate
- Lethargy
- Progressive loss of consciousness
- Progressive memory loss
- Subtle personality changes
Additionally, patients may exhibit:
- Dementia
- Loss of ability to speak or swallow
- Muscle atrophy
- Myoclonus – involuntary muscle twitching
- Nystagmus – rapid involuntary eye movement
- Seizures
- Tremors
What is Metabolic Encephalopathy?
Metabolic encephalopathies (MEs) are a set of neurological disorders caused by underlying systemic illness. There are two broad categories of metabolic encephalopathies: 1) resulting from lack of glucose, O2 or metabolic factors, and 2) due to peripheral organ dysfunction:
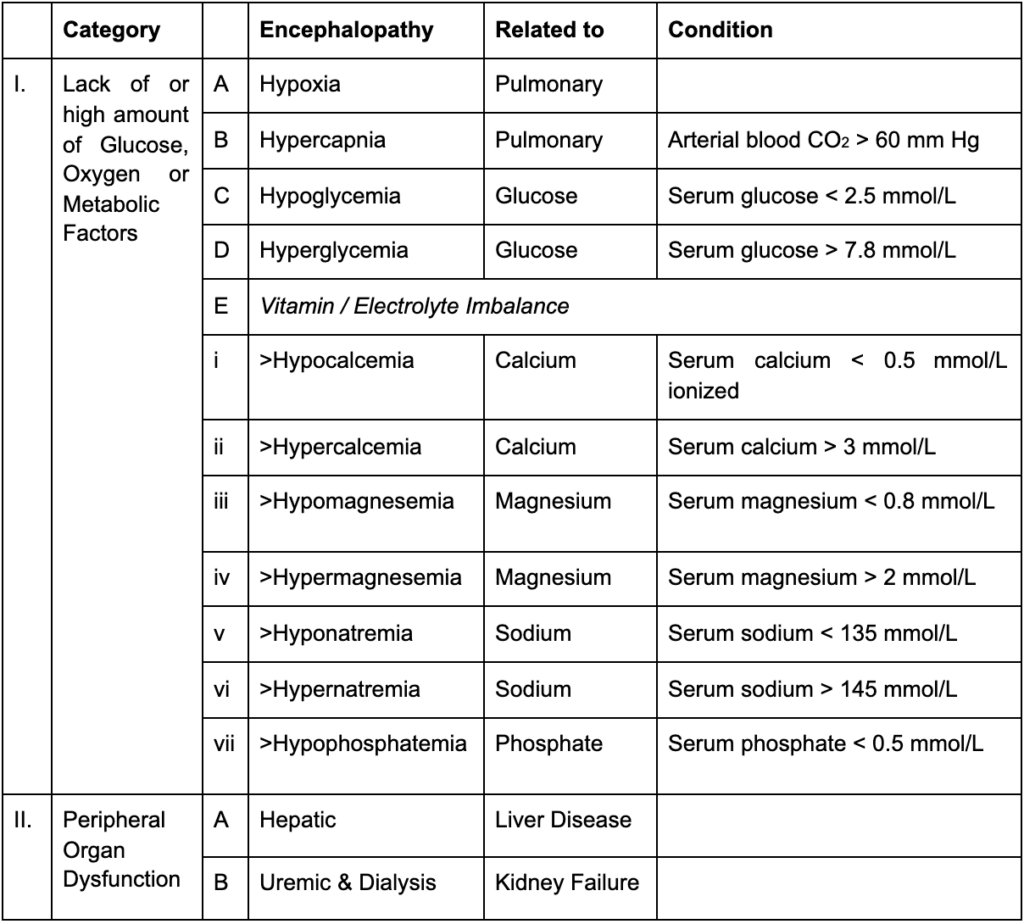
Note: Serum – blood; above table is not exhaustive
Diagnosis
Diagnosing metabolic encephalopathies can be tricky due to patients presenting with a range of symptoms. Encephalopathies are symptomatic of an underlying condition, so tests must be conducted for the illness in addition to the patient’s neurological condition. The combination of tests most commonly used are blood tests (for ammonia levels and toxin content), magnetic resonance imaging (MRI) and electroencephalogram (EEG). Additionally, patients’ cognitive function (sensory and motor skills) are tested to discern the current stage of disease.
The most common metabolic encephalopathies, their causes, symptoms and treatment are outlined below:
1. Type – Hypoxic & Hypercapnic encephalopathies arise due to insufficient respiration. The most common cause is excess CO2 retention, which causes CNS disturbance. CO2 is a part of our metabolism, however, it is toxic at elevated levels. Hypoxia is defined as when there is insufficient O2 supply, in this case to the brain. These conditions are worsened by underlying infection or congestive heart failure.
Causes – Hypercapnia is the result of an acute metabolic, pulmonary or cardiac failure resulting from chronic pulmonary disease such as bronchitis.
Hypoxemic chronic obstructive pulmonary disease (COPD) is a condition where alveoli and then other parts of the lungs receive insufficient O2.
Symptoms – Headache; ataxia (loss of control of body movements); reduced vigilance; inattention; confusion; drowsiness; memory loss; asterixis; myoclonus; stupor & coma.
CMR (GLC) decreases as a result of decreased neuronal activity and therefore brain glucose requirement.
Treatment – Correction of CO2 and O2 levels result in recovery.
Patients with COPD usually are treated with continuous O2 supply and show improved cognitive and motor skills.
2.Type – Hypoglycemia is a condition whereby glucose level in the bloodstream is reduced. As the brain primarily uses glucose as fuel, areas of higher function that have a higher metabolic demand are more susceptible to hypoglycemia. During hypoglycemia, CMR (glc) falls more rapidly than CMR (O2), causing the brain to use substrates other than glucose. These substrates can sustain cerebral function for only a few minutes, after which brain damage occurs.
Causes – The population at higher risk:
age 65+
previous hypoglycemic episodes
low haemoglobin
pre-existing conditions – kidney / heart disease
patients with type one diabetes or reduced C-peptide levels
Symptoms – Cold perspiration; tachycardia; light-headedness; headache & mild agitation.
Severe seizures; cerebral edema & hypoxia.
Symptoms mimic stroke.
Treatment – Requires sustained therapy, continuous administration and monitoring of glucose levels. Insulin overdose requires a diluted glucose solution.
Glucagon (the hormone that raises blood glucose levels) can be administered in extreme cases.
3.Type – Hyperglycemia occurs due to high blood glucose levels.
It is a result of reduced insulin secretion, decreased glucose utilisation and increased glucose production.
Left untreated, hyperglycemia can cause damage to the eyes, kidneys, heart, nerves and peripheral vascular system.
Causes – This usually occurs in at-risk populations during severe metabolic stress, such as infections, burns, inflammatory diseases or steroid use. Can also occur spontaneously.
Symptoms –
Polyuria – diluted urine
Polydipsia – abnormally high thirst due to disease
weight loss
Treatment –
I – fluid replacement
II – intravenous insulin therapy
III – potassium replacement
IV – close electrolyte monitoring
V – lifestyle changes – diet and physical activity
4.Type – Hepatic encephalopathy is classified as either acute or chronic resulting from underlying liver disease. The exact physiology is not known, however, an indicator is increased arterial and brain ammonia. After being absorbed by the gut, ammonia travels to the liver for detoxification. Liver dysfunction increases arterial ammonia. As it navigates its way to the brain, ammonia enhances γ
-aminobutyric acid transmission. γ
-aminobutyric acid is an inhibitory neurotransmitter.
Causes – Viral hepatitis (causes liver inflammation & damage), drugs, toxins, liver cirrhosis, vascular disease, Wilson’s disease (non-alcoholic liver cirrhosis), lymphoma, Reye syndrome & acute fatty liver of pregnancy.
Symptoms –
Stages:
I – inattentive, irritable, impaired visual and motor skills, tremor, myoclonus, asterixis*
II – blunted attention, lethargy, anxiousness, delirium
III – stupor but rousable, impaired cognition, nystagmus
IV – coma, spasticity, nystagmus
Treatment –
I – treatment of any infection
II – reversing triggers (such as internal bleeding)
III – restriction of protein intake
IV – address ammonia imbalance (lower arterial ammonia, lactulose – increases uptake of gut ammonia so it passes through the stool)
If all the above fail, and the condition advances, the only remedy is a liver transplant.
5.Type – Uremic encephalopathy is associated with loss in the kidney’s ability to perform its normal functions – eliminating waste from the body’s blood, and secretion of hormones. Uremia, a condition where the bloodstream contains high levels of uric acid and nitrogen compounds, makes its way through the bloodstream up to the brain, causing encephalopathy. Compounds include guanidine compounds, parathyroid hormone, urea and middle molecules.
Causes – Accumulation of neurotoxins that inhibit proper cognitive function.
Symptoms –
Acute
Reduced attention; impaired construction & writing; executive dysfunction; behavioural changes; sleep disturbances; agitated delirium; seizures & coma
Chronic
Slowness of thought; headache; apathy; inattention; impaired construction; myoclonus, asterixis*
Treatment –
I – treatment is first administered to relieve symptoms
II – dialysis is used in cases of renal failure
III – failing the above, a kidney transplant may be required
Note: Myoclonus – involuntary twitching of muscles; Asterixis – periodic loss of muscle tone.
Acute Toxic Metabolic Encephalopathy
Acute toxic metabolic encephalopathy (TME) is a broad term used to describe a condition of global cerebral dysfunction. TME is a non-traumatic acquired brain injury, with symptoms that include altered consciousness, behavioural changes and seizures. TMEs are not related to cerebral dysfunction resulting from structural abnormalities, primary brain disease, immune-mediated inflammation or CNS infection.
Conclusion
Our brain modulates and regulates thousands of functions across our bodies. It depends on an uninterrupted supply of nutrients for proper functioning. Encephalopathies are a group of disorders of the brain that vary widely by cause and symptoms, ranging from a headache to coma. Encephalopathies lead to impaired brain function. They can either be reversible or irreversible. The severity of encephalopathy depends on the period before diagnosis and the damage that has already been done. Early detection and timely intervention can significantly improve patient outcomes. Metabolic encephalopathies (ME) are unrelated to structural damage, resulting from underlying systemic illnesses that eventually affect the brain. Lack of glucose, oxygen and other metabolic factors contribute to ME. Acute toxic metabolic encephalopathies, as the name suggests, relates to toxins not being properly disposed of by the body during its normal metabolism. These toxins enter and wreak havoc on the brain. It is thus important to get regular checks done and visit a doctor if symptoms present themselves.
Disclaimer:The contents of this article are for general information and educational purposes only. It neither provides any medical advice nor intends to substitute professional medical opinion on the treatment, diagnosis, prevention or alleviation of any disease, disorder or disability. Always consult with your doctor or qualified healthcare professional about your health condition and/or concerns and before undertaking a new health care regimen including making any dietary or lifestyle changes.
References
- https://journals.physiology.org/doi/full/10.1152/physrev.00062.2017
- https://www.ncbi.nlm.nih.gov/books/NBK28194/
- https://accessanesthesiology.mhmedical.com/content.aspx?bookid=1750§ionid=117318875#:~:text=BRAIN%20METABOLISM,-%2B%2B&text=Cerebral%20metabolic%20rate%20(CMR)%20is,min%20in%20the%20resting%20state.
- https://www.ninds.nih.gov/Disorders/All-Disorders/Encephalopathy-Information-Page
- https://www.webmd.com/brain/what-is-encephalopathy